
The left ventricle decompensated by the use of a suction which inserted through fossa ovalis. At 28 ✬ the aorta was clamped and blood cardioplegia was administered to the aortic root, and direct cardioplegia was repeated in every 20 minutes. During cooling period, pulmonary trunk was separated from ascending aorta, right and left pulmonary arteries were dissected out to their first branches. Ascending aorta was cannulated just below the truncus brachiocephalicus. After proper stabilization, patient was repositioned for the second incision and midline sternotomy was performed. After completion of anastomosis, vascular clamps were removed and thoracotomy was closed in a routine manner. The two vascular clamps were then approximated allowing proximal and distal segments to be anastomosed using 7-0 polyprolene suture without any tension. An incision was performed in proximal clamped area and elongated to the under surface of the left subclavian artery. Following transsection of descending thoracic aorta, all ductal tissue was completely excised from the distal segment of aorta. A part of origin of left subclavian artery was included within the proximal site. Thoracic aorta and distal archus aorta were clamped using side clamps. PDA was ligated and PGE1 infusion was stopped. Topical hypothermia was achieved at 34 ✬. Large and multiple collateral vessels were observed. Descending thoracic aorta was mobilized down to the diaphragm. Aortic segments, pulmonary artery and arch vessels were all identified and extensively mobilized without damaging or sacrifying any intercostal arteries. A left posterolateral thoracotomy was performed and thorax was opened through the fourth intercostal space. Surgery was performed three days following the admission due to the elevated indirect bilirubin levels.įig 1: Preoperative aortogram showing (a) type A aortic arch interruption, (b) a collateral artery originating from ascending aorta supplying descending aorta. Pulse oxymetry saturation was 65% and no acidosis was detected. 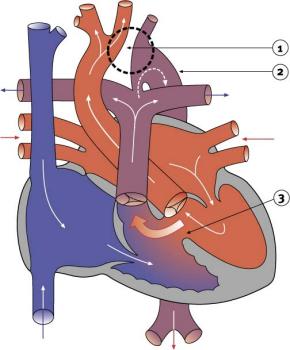 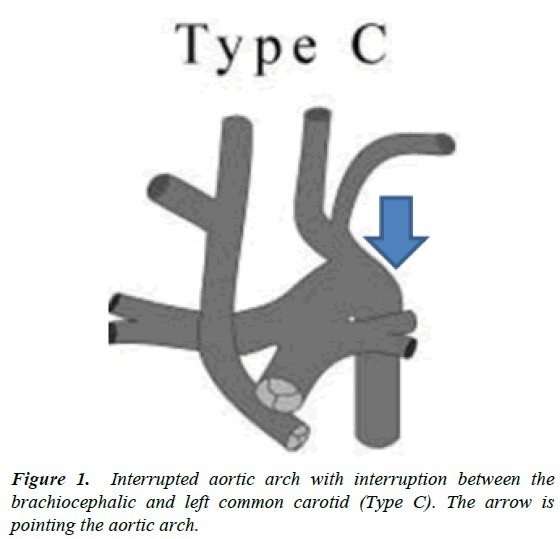
Balloon atrial septectomy and selective angiocardiography were performed (Fig. Echocardiographic examination demonstrated TGA with anteroposterior position of the great arteries, narrow Patent Ductus Arteriosus (PDA) and aortic arch interrupted distal to the left subclavian artery (IAA, type A). All rights reserved.A 6-days-old cyanotic male neonate, weighing 3.5 kg was admitted to our institution with a prostaglandin infusion. Published by MMCTS on behalf of the European Association for Cardio-Thoracic Surgery. We also briefly discuss stage 2 of the repair, which is a straightforward VSD closure and pulmonary artery debanding procedure when the child is older and more resilient. This approach significantly reduces morbidity and results in a well-palliated ventricular septal defect (VSD). 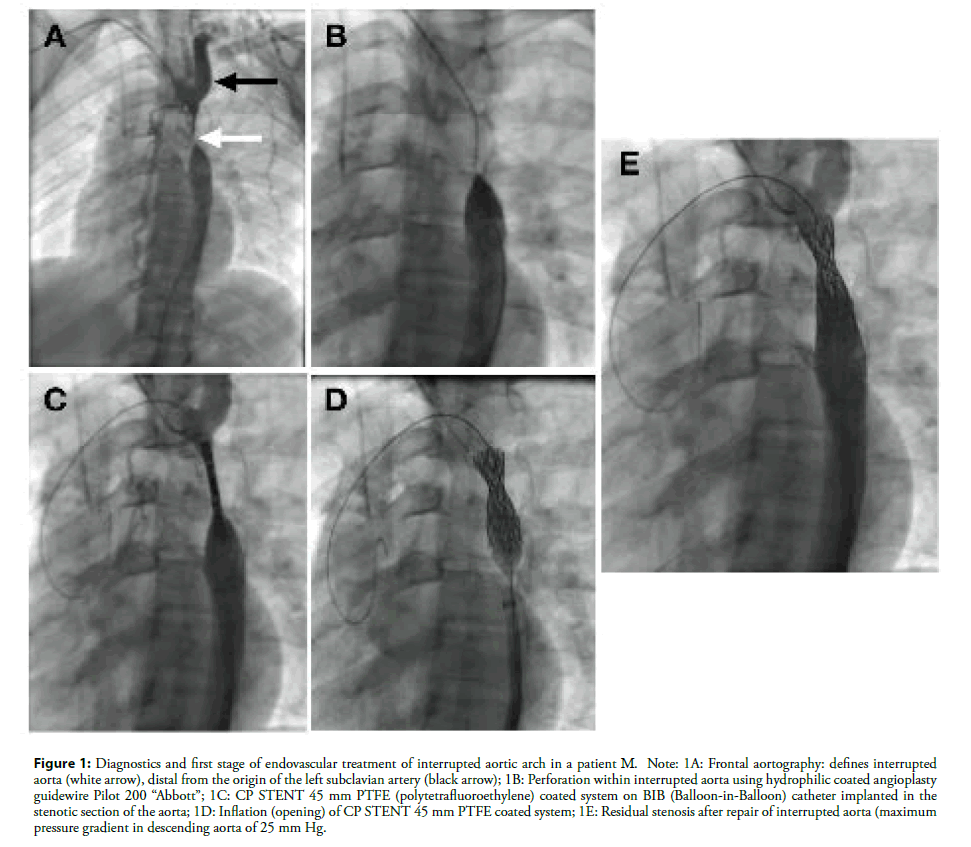
Key steps of stage 1 repair are demonstrated and the arguments supporting our approach are presented. In this video tutorial, we demonstrate our preferred technique for neonatal aortic arch repair and pulmonary artery banding, which constitute the first stage of the 2-stage repair. While palliation, in general, has fallen out of favor, a 2-stage approach to correcting selected type A IAA appears to be a productive, safe, and effective option, considering the neonatal age at repair. Single-stage complete repair has become the norm in contemporary practice. Treatment of interrupted aortic arch (IAA) is inherently challenging.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
